Project Lead(s): John Quinn
Issue
Access to quality diagnostics is a critical health challenge in Uganda and other developing countries.
In many low-income settings, misdiagnosis of diseases such as malaria and tuberculosis (due to a lack of capacity to examine samples microscopically) has caused high fatality rates, drug resistance, economic burden and eroded trust of local medical practitioners.
Recent innovations in mobile phone camera-based microscopy have opened up an entirely new way to diagnose infectious diseases remotely.
Solution
The hypothesis tested by the project was that recent advances in hardware fabrication and artificial intelligence software could be used to attach a mobile phone to a camera and to create effective diagnostic tools for common tropical conditions, such as malaria.
The project aimed to exploit the relatively widespread availability of microscopes (present in 50% of rural Ugandan health facilities, even though only 17% of health facilities have laboratory technicians who can operate them) and widespread access to increasingly powerful smartphones.
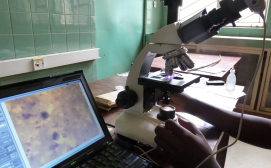
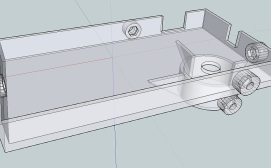
Customized, low-cost adapters were created with 3D printing and used to mount smartphones on microscopes. This technology provides an opportunity to create one-off customized adapters for any camera phone and microscope combination and dramatically reduces the development costs for new products, as well as allowing rapid prototyping capabilities and easy repair.
The software component uses deep-learning techniques to effectively identify pathogens. Three unique diagnostic datasets, composed of annotated images for plasmodium, tuberculosis bacilli and intestinal parasite eggs, were collected and are now available online.
The team focused on the diagnostic abilities of this new approach for malaria (in blood samples), tuberculosis (in sputum samples) and intestinal parasites (in stool samples).
Outcome
The team successfully developed an adapter for mounting a mobile phone onto a microscope for the remote diagnosis of common infectious diseases.
Using the performance measure of average precision (AP) with a scale of 0 (worst) to 1 (best), they found the diagnostic ability of the tool was 0.97 for malaria, 0.93 for TB and 0.93 for intestinal parasites.
These strong results constitute evidence that this approach could be the basis of an effective fully- or semi-automated, point-of-care diagnosis system.
This work has not been directly applied to diagnosis of individuals, but the materials developed and analysis undertaken by the team have brought this possibility within reach.
The next stage for the project would involve clinical trials, prior to marketing and commercialization of the hardware/software platform.