Guest blog by Samara Everman, Global Social Impact Fellow

High maternal mortality rate in Sierra Leone
Sierra Leone has one of the world’s highest maternal mortality rates, with 1,360 deaths per 100,000 live births. Often, mothers do not have the disposable income or time required to travel long distances to health facilities. Consequently, women wait until their condition becomes life-threatening. At the health facility, women face various challenges associated with a reduced supply of medical resources and the trained personnel required to use them. This can be avoided if patients are screened and routinely tested for common maternal conditions such as Urinary Tract Infections (UTIs) or Preeclampsia. UTIs are the most common bacterial infection among pregnant women and can lead to a myriad of complications, including kidney damage, sepsis, and maternal mortality. Similarly, Sierra Leonean mothers are rarely screened or diagnosed for preeclampsia, a hypertensive condition that commonly develops during pregnancy and can progress into eclampsia, causing postpartum hemorrhage or death. Although preeclampsia and UTIs can be easily diagnosed, the economic and geographical barriers in Sierra Leone block mothers from tests and treatment.
Our solution
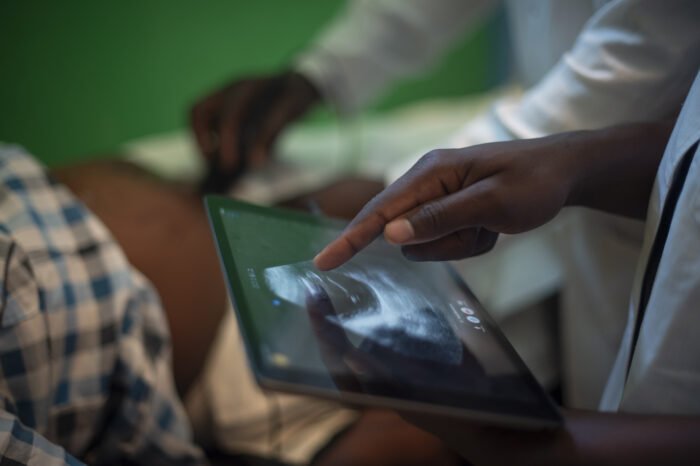
What if a product screened women for preeclampsia and UTIs in the comfort and privacy of their own homes? Lehigh University and World Hope International Inc. introduced Ukweli Test Strips to the Bombali district of Sierra Leone in 2019. Ukweli Test Strips is a low-cost three-parameter urinalysis test strip to screen women for UTIs and preeclampsia across the healthcare system. Currently, there is a nine-parameter test strip that is both unaffordable ($2.00/strip) and demands a high level of education to interpret. Ukweli simplifies the existing nine-parameter test strip to three parameters. Ukweli is specific to preeclampsia and UTIs, affordable costing $0.20 per patient and accessible for the women in Sierra Leone with an option to receive testing in the comfort of their homes by trusted community health workers. Screening pregnant women early and often through Ukweli Test Strips can be fundamental to change. After being screened, the woman can know whether she needs to make the journey to see a doctor or if she is healthy. Currently, over half a million people have access to Ukweli Test Strips, and this would not be possible without the generous support from Grand Challenges Canada!
So, how did we get to this point, and how did the women respond to Ukweli?
Irrespective of the technology, the Ukweli Team needed to be attuned and responsive to the consumer and market needs in an ever-changing environment. The Stars in Global Health grant of $100,000 enabled Gabrielle Gundermann, a member of the Ukweli team, to conduct a pilot study in Makeni, Sierra Leone that investigated the various distribution and messaging methods. The primary goal of the six-month study was to determine the willingness of patients to get screened for UTIs and preeclampsia and pay for screening at 14 different healthcare centers. Funding from Grand Challenges Canada not only helped Ukweli determine the best way to help pregnant women get screened but was used to screen 2,789 pregnant women for UTIs and preeclampsia, of which 282 women received a relevant referral from trained community health workers. To ensure the study’s validity, Gundermann served as a liaison between the Ukweli team and several Peripheral Health Units in Sierra Leone, which was particularly helpful in building long-lasting partnerships.
In 2010, Sierra Leone’s Free Health Care Initiative was established and covered the health care needs of children under five and pregnant and lactating women. While care is free for patients that meet the criteria, the policy does not cover the cost of drugs, treatment, or screening for illnesses or diseases. The Free Health Care Initiative was an important factor in contributing to improvements in coverage equity of essential services for mothers and children; however, its nuances impacted the development of Ukweli’s business model. The venture also partnered with the Sierra Leone Ministry of Health, the country’s Pharmacy Control Board, and the Community Health Workers (CHWs) specific to local health clinics.
The Ukweli team has engaged its government partners to obtain licensing and marketing rights. The following 3 phases advanced the team to get Ukweli Test Strips to women in need.
Ukweli significantly built off of the Grand Challenges Canada-funded pilot study. Transitioning from the research study into the implementation and distribution of these test strips is proof of the venture’s commitment to scale into the Sierra Leone health care system and reach the vulnerable women in need.
1. Approvals: Pharmacy Control Board and Service Level Agreement
The first step to getting Ukweli Test Strips in Sierra Leone was to submit an application to The Pharmacy Board of Sierra Leone. The application required documents regarding manufacturing procedures, stability data, sterility certificates, and analytical control procedures performed on the product. We aligned the products’ packaging to the existing labelling regulations of the Pharmacy Board and worked with the OEM to secure the forms necessary to ensure the approval. As of Oct. 16, 2019, Ukweli Test Strips is a registered medical device, able to be sold and marketed in Sierra Leone with a Pharmacy Control Board
license.
From the beginning, Ukweli set out to seamlessly integrate its product into the healthcare system in Sierra Leone. This required a Service Level Agreement with the Ministry of Health and Sanitation. After several negotiation meetings, the Ministry of Health and Sanitation granted the venture a service level agreement to market and sell our strips through official health facilities. As of April 2020, the team can leverage the Community Health Network to sell test strips. Ukweli’s innovation is not in the technology; what makes this venture particularly novel is how it addresses last-mile distribution challenges.
2. Addressing the last-mile distribution challenge
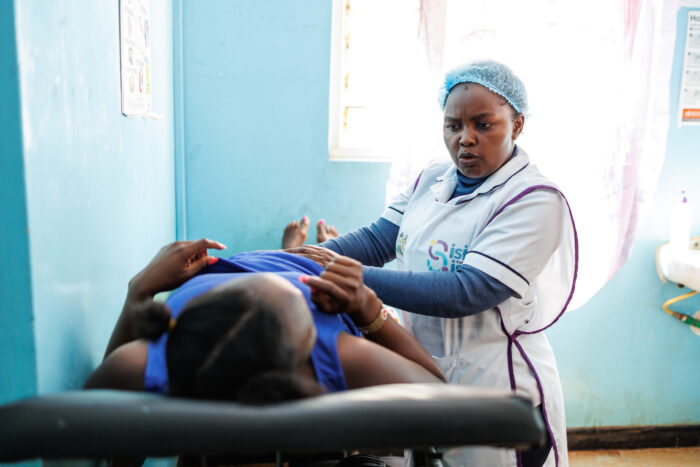
Once the Sierra Leonean Pharmacy Board and the Ministry of Health granted their respective approvals, the Ukweli team utilized the results from the pilot study, which discovered an optimal pricing strategy: charging 2,000 Leones ($0.20) for each test strip and working within the Community Health Network. This may seem counterintuitive given Sierra Leone’s free health care mandate; however, women pay for the product, not the service. The study’s results indicated that $0.20 is optimal based on the willingness to pay for the strip. Ukweli prioritizes screening individuals in the comfort of their own homes. To do so, the test strips are distributed to trusted CHWs at Peripheral Health Units.
To get the strips into the Peripheral Health Units, Ukweli’s distribution strategy relies on two Distribution Managers: Jawara Koroma and Hassan Mahamed Soio. They onboard Peripheral Health Units and train the Community Health Workers to become Ukweli-Certified. In the four-hour training workshop, the distribution managers educate the health workers on UTIs and preeclampsia, appropriate use of the test strip, informed consent, and the protocol to take while referring a patient. Jawara and Hassan sell the boxes containing 100 strips to the new Ukweli Certified Health Workers for 50,000 Leones per box. To encourage the Ukweli Health Workers to conduct screenings regularly, they charge women in their community for each test strip – this allows each Ukweli Health Worker to earn back the cost of their test strip purchase and a profit while simultaneously referring women who screen positive for UTIs or preeclampsia to an appropriate healthcare facility for treatment. Ukweli Health Workers and distribution managers have a high level of agency, meaning operations are significantly hands-off for Lehigh’s team. Each step of the Ukweli business model is reliable and repeatable, and it has proven to be successful with the onboarding of 56 Peripheral Health Units to date.
3. Building data infrastructure to facilitate scale
The Distribution Manager collects screening data from each Peripheral Health Unit integrating data into a centralized Ukweli database. The Peripheral Health Units’ data can be visualized using the interactive ArcGIS Mapping Software – this allows the user to analyze the data and see the geographic distribution of Ukweli Test Strips activity. While the overarching goal is to reduce Sierra Leone’s maternal death rate, this is difficult to quantify. Key indicators tracked by the team include the number of boxes sold, Peripheral Health Units onboarded, CHWs trained, and women tested. The data dashboard is effective in monitoring and evaluating stakeholder interaction with Ukweli and identifying any changes to operations.
Thanks to Grand Challenges Canada, Ukweli is changing how pregnant women in Sierra Leone monitor their health without disrupting the current health-care system. Now, women are able to get screened for UTIs and preeclampsia in the comfort and privacy of their own homes. The pilot study enabled Ukweli to screen women in the targeted communities and save lives. Integrating a dependable and sustainable business model can be onerous for early-stage ventures; we anticipate these insights into our journey to guide new social and business innovations.