This blog is crossposted from the Mental Health Innovation Network website. The original blog by Agnes Becker, Targeted Communications Manager at the London School of Hygiene and Tropical Medicine and the Mental Health Innovation Network, can be found here: ‘Friendship Bench’ tackles mental health and HIV in Zimbabwe and beyond.

“It was so hard for me. Before the Friendship Bench I really struggled.”
– Mrs Wyeni, service user“[Through the Friendship Bench] I learned that I can fix my problems with support from my family.”
– Mrs Munyaradsi, service user
Sitting under a tree next to the Western Triangle clinic in the outskirts of Harare, Zimbabwe, it’s hard to imagine that the joyous circle of singing and dancing women and men around me were once so desperate, many attempted suicide. In the centre of the circle, crafted out of wood and covered in crocheted bags, baby clothes, glassware, polish and spices, is the reason for their recovery: The Friendship Bench.
How the Friendship Bench improves mental health and HIV
“The integration of mental health into other programmes, like HIV, can improve these programmes.”
– Dr David Okello, WHO Representative, Zimbabwe
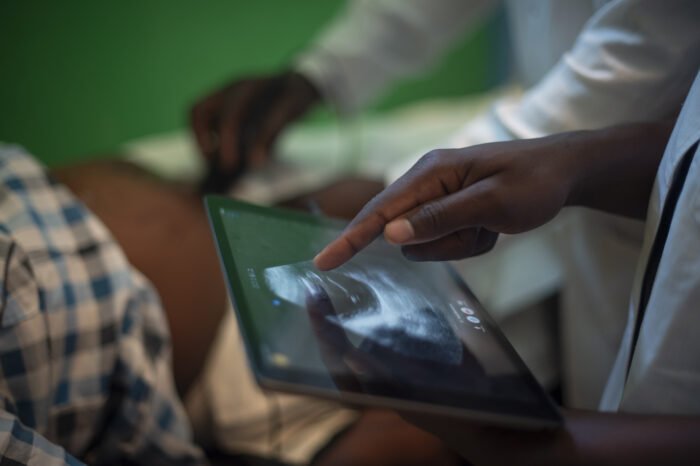
Research has identified close links between mental illness and chronic diseases like HIV/AIDS. Common mental disorders associated with Shona concepts of kufungisisa (thinking too much), kusuwisisa (deep sadness), and moyo unorwadza (painful heart) are prevalent among the 15% of adults in Zimbabwe who are currently living with HIV/AIDS. Because people living with mental health problems are less likely to adhere to the HIV anti-retroviral treatment, it is important for countries like Zimbabwe to provide mental health care alongside HIV/AIDS services.
However, Zimbabwe faces a critical shortage of mental health specialists with only 12 psychiatrists serving a national population of 15.3 million. The Friendship Bench, a mental health project led by Dr. Dixon Chibanda from the Zimbabwean AIDS Prevention Programme and supported by Grand Challenges Canada (funded by the Government of Canada), tackles this problem by training lay health workers to counsel people with common mental disorders in primary care clinics.
“Before Friendship Bench my counselling was to say “do this and do that”. Now I learnt that is not the way. I must ask them…to open their mind. To fix their own problems. To learn this for themselves. I see how it helps them. I think this bench should not just grow to all Zimbabwe. It should go to all the world.”
– Shekede, lay health worker or ‘Grandmother’
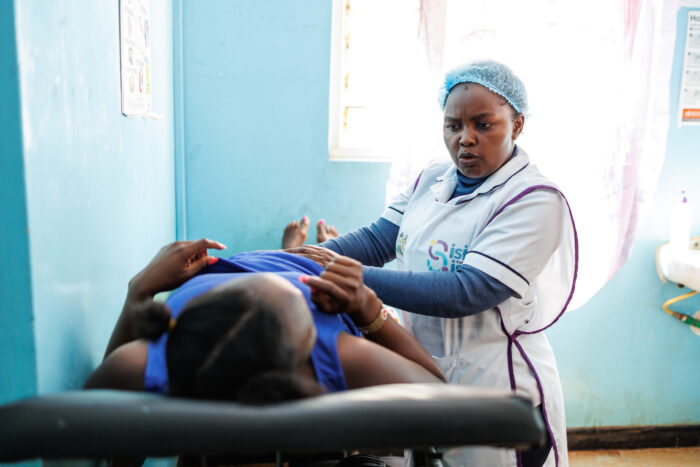
Benches are placed outside clinics where people come to access services for a variety of health conditions, including HIV/AIDS. Lay health workers, known as Golden Ladies or ‘Grandmothers’, are trained to offer problem-solving therapy to people who are referred to the benches by clinicians. They receive up to six counselling sessions with the Friendship Bench Grandmothers, including one home visit and, in some cases, referral to other health or social services, or income-generating activities. The handmade bags and baby clothes, and the polish and glassware lying on the bench are sold by Friendship Bench service users for income, providing vital cash to help lift them out of poverty.
I’d read about the project before, but it wasn’t until I sat under that tree, listening to testimony after testimony that I realized just how much of an impact such a simple intervention can have:
There was a woman who became depressed when she had to conceal from her husband the child she had given birth to after being raped by her father’s friend. She spoke about how the Friendship Bench Grandmother’s counselling helped her to tell her husband and, with his support, confront and forgive the man who raped her.
One man spoke about how his depression and hatred for women spiralled out of control after he contracted HIV from his wife who had not told him her HIV status. The Friendship Bench helped him through his depression and hatred and he is now able to have good relationships with women again.
Another woman had become so depressed she considered killing her children. She tried to commit suicide by eating 7 packets of poison and her stomach is now permanently perforated from the damage. Through the Friendship Bench she is now back to work selling spices; she is also expecting her second child.
The stories made me think of friends at home who also battle with depression, some as a result of sexual assault. Mental health is something that affects us all.
Working together for sustainability
A pilot study in 2006 showed clinically meaningful improvement in symptoms of common mental disorders among recipients of the Friendship Bench innovation in three clinics in Mbare, Harare. A recently concluded Randomized Controlled Trial is providing further evidence for this impact – with published results expected in 2016. The project is now considering how to make their innovation sustainable.
I was visiting the Friendship Bench as part of a Mental Health Innovation Network country support visit, in partnership with the Overseas Development Institute (ODI). The reason for our visit? To encourage stakeholder engagement with the project and run a workshop, funded by Grand Challenges Canada, with the Friendship Bench team and their partners on preparing for scale and sustainability. During the workshop we used the ODI ROMA Global Mental Health Policy Influence Toolkit, the MHIN Global Mental Health Communications Toolkit and case studies of scale up from other contexts
The enthusiasm during the workshop was infectious – we even came up with 2 minute pitches to key stakeholders:
https://www.youtube.com/watch?v=Fyoqa93e8Nk
Mental health in Zimbabwe: What’s next?
The last day of the workshop saw the coming together of The Friendship Bench, Médecins Sans Frontières, Harare City Health Department, the Ministry of Health, Zimbabwe’s Provincial Medial Directors and the WHO country office. Having such an influential group of stakeholders in the room talking about mental health was a first in Zimbabwe. The group identified 6 priority areas for all partners to improve mental health services in Zimbabwe:
- Awareness and sensitisation for health policy and planning officials, service providers and the population
- Integrating mental health into other health sectors, such as HIV
- Good quality support and supervision of service providers
- Gradual scale up of health services, such as the Friendship Bench
- Collaboration between government, business, NGOs and service providers
- Ensuring the sustainability of mental health services, such as the Friendship Bench
“I was convinced that this bench works. We don’t have anything cheaper. We don’t have the psychiatrists in Harare. This bench is filling that gap…It’s a cheap way. It’s an effective way…It must be replicated in other cities and provinces in the region.”
– Dr Prosper Chonzi, Director of Health, City Health Department, Harare, Zimbabwe
My trip to Zimbabwe has been eye-opening. Seeing the reality of a project on the ground – how such a simple concept can help people to find hope again – was moving. The success of the Friendship Bench is bringing partners together to think about how to scale up to other areas in Harare and beyond.
To learn more about the Friendship Bench project, visit their project page on the Mental Health Innovation Network website.
We encourage you to post your questions and comments about this blog post on our Facebook page Grand Challenges Canada and on Twitter @gchallenges.