Erica McKenzie is Bhutan Epilepsy Project researcher who works with Principal Investigator Farrah Mateen MD, PhD, based at the University of Ottawa, Massachusetts General Hospital/Harvard Medical School, and the JDWNR Hospital in Thimphu, Bhutan. Erica is a medical student at Queen’s University in Kingston, ON.
Walk the streets of Thimphu, the capital of Bhutan, and you will encounter Buddhist monks draped in floor-length red and orange robes, chatting away with ears pressed to cellphones. In this remote Himalayan kingdom, the modern coexists with the traditional. This is especially true of healthcare in Bhutan, where modern medical treatment is accessed alongside traditional Buddhist therapies, and time-honoured cultural beliefs about illness coincide with the enthusiastic uptake of new health technologies.
The geographic, economic, and cultural landscape of Bhutan poses several challenges to the effective treatment of complex health issues like epilepsy. No neurologists and fewer than 200 allopathically trained physicians practice in Bhutan. Epilepsy referrals are primarily handled by the sole department of psychiatry, based out of Jigme Dorji Wangchuk National Referral (JDWNR) Hospital in Thimphu. Most of Bhutan’s 700,000 people live in rural areas, and Thimphu is days of travel by foot or bus for many patients from remote villages. Limited resources prevent the adoption of costly diagnostic technologies such as standard electroencephalogram (EEG) machines, which monitor brainwaves and are a standard of epilepsy diagnosis in the developed world. Finally, traditional beliefs cast epilepsy as a contagious or spiritual affliction, leading to stigma against those with epilepsy and reluctance to seek care for seizures.

One project is using a cutting edge smartphone-based EEG to tackle the difficulties of caring for those with epilepsy in Bhutan. The Bhutan Epilepsy Project received a seed grant in the Global Mental Health program from Grand Challenges Canada, funded by the Government of Canada, and additional funding from the Thrasher Foundation. The project is a collaboration between the department of psychiatry at the JDWNR in Bhutan, the Massachusetts General Hospital, the Massachusetts Institute of Technology, the University of Ottawa and the Technical University of Denmark. Researchers aim to assess the feasibility of using the new technology to diagnose and monitor epilepsy, while also building knowledge about the medical, social, and cultural features of epilepsy in Bhutan.
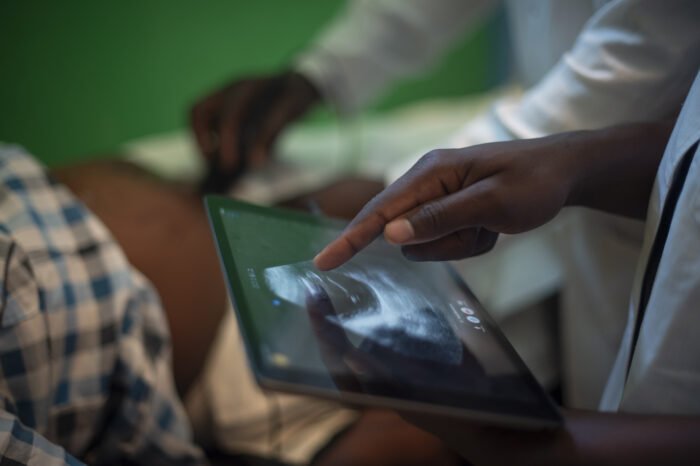
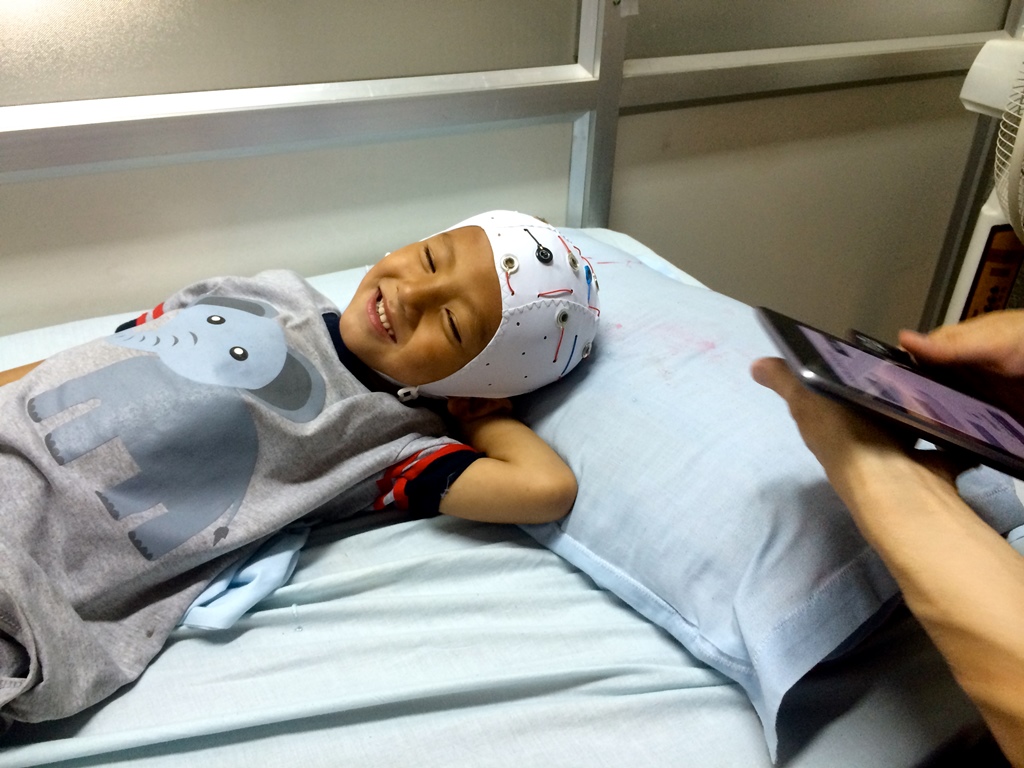
The smartphone EEG is an elegant solution to a complex problem. The device, developed by Arkadiusz Stopczynski at the Technical University of Denmark, uses open-source software and the computing power of commercially available mobile devices to wirelessly record brainwaves transmitted from an electrode cap. The setup costs less than $500, compared to tens of thousands of dollars for a standard EEG machine, and is highly portable, inviting the possibility of bringing the smartphone EEG to the patient’s doorstep. The smartphone EEG is easy to use: unlike a standard EEG, which requires the application of dozens of individual wires and electrodes by a specialized technician, it can be operated successfully by community health workers with only basic training. The device can wirelessly transmit the EEG recordings over long distances, allowing the epilepsy expert interpreting the recording to be located anywhere in the world.
The Bhutan Epilepsy Project began recruitment in July of 2014, and the response from the community was nearly overwhelming: subjects traveled from the farthest provinces of Bhutan to participate and crowded the halls of the Psychiatry Department of the JDWNRH. Among the first participants to enroll was Pema Tshering (*), a young Bhutanese woman with epilepsy. Pema had previously sought traditional therapies for her seizures, and arrived for her visit bearing small circular burns on her scalp and back, a vestige of a Buddhist treatment that involves applying fire-heated coins to the skin in an effort to relieve the seizures.

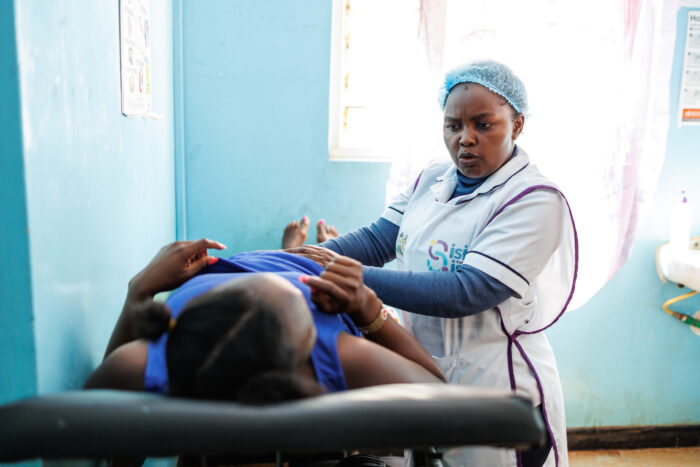
Pema, like each of the Project’s participants, completed a clinical interview and series of questionnaires on the clinical features of her epilepsy, her quality of life, her understanding of epilepsy, and her experience of epilepsy stigma. She received a smartphone EEG and a standard EEG, and her recordings were transmitted to an epilepsy expert at the Massachusetts General Hospital. She also received an MRI scan and testing for neurocysticercosis, an infectious parasite. At the end of this workup, Pema and her health care team were armed with key information about her epilepsy syndrome, and able to tailor her treatment based on this enhanced diagnostic information.
To date, more than 200 participants have been enrolled in the Bhutan Epilepsy Project. While the study is ongoing, we are excited to share some early insights from the project:
Current epilepsy management in Bhutan is inadequate;
- 60% of participants had experienced a seizure in the past month, despite 90% of participants being treated with anti-epileptic medications
- 27% of participants had experienced seizure-related accidental injuries, including car accidents, burns, and fractures
Cultural beliefs about epilepsy influence the patient experience;
- 48% of participants reported believing that karma or actions in one’s past or current life could cause epilepsy
The project will continue to grow in 2015. Recruitment continues at the JDWNRH in Thimphu, and next steps will involve implementing the smartphone EEG at community health posts in rural Bhutan. Educational outreach aimed at reducing the stigma of epilepsy is already underway. Merging cutting edge diagnostic technology with culturally aware education, the Bhutan Epilepsy Project hopes to take the best of the traditional and the modern to improve the lives of those with epilepsy in Bhutan.
Additional Links:
We encourage you to post your questions and comments about this blog post on our Facebook page Grand Challenges Canada and on Twitter @gchallenges.