Dr Nitika Pant Pai is an Assistant Professor in the Department of Medicine (Divisions of Clinical Epidemiology and Infectious Diseases), at McGill University and McGill University Health Center, Montreal, Canada. She is a Grand Challenges Canada Grantee in the Stars in Global Health (Round 1) Program.
Today, December 1, 2013, is ‘World Aids Day’. HIV is not a death sentence as it was thirty years ago. The advent of highly active Antiretroviral therapy (ART) has made it a chronic manageable disease. However, an early initiation of ART controls HIV effectively and reduces transmission of the virus to partners and children,. Since mid 2000s ART is universally available in low- and middle-income countries. The challenge now is to find people who are infected, but don’t know their serostatus and bring them into treatment so that we achieve the vision of zero HIV infection. We believe that expanded access to HIV testing can help in this regard.
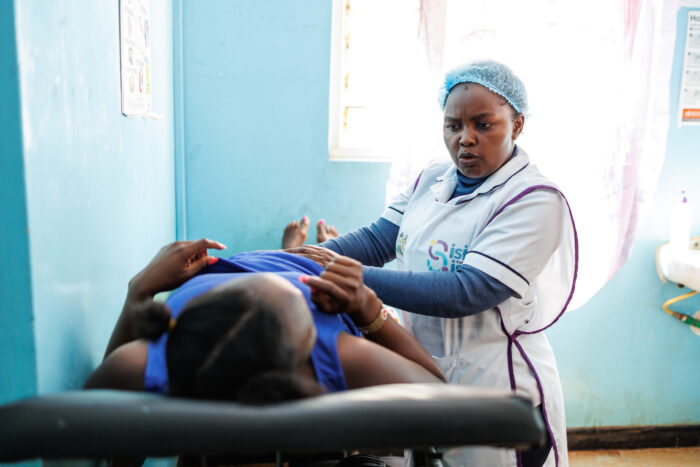
 HIV testing is the cornerstone of prevention and treatment. Current model of HIV testing is based on people showing up in health care facilities to test. Many (this includes men more than women) avoid testing in health facilities because of social visibility, privacy concerns, fear of lack of confidentiality, stigma, discrimination, and also long waiting time, that results in loss of work days. Is it any surprise that 60% of the people living with HIV don’t know that they are infected and continue to spread the infection to their unsuspecting sex partners and children. For those who are tested in facilities, about 30-50% do not return to know their results and never get linked to care.
HIV testing is the cornerstone of prevention and treatment. Current model of HIV testing is based on people showing up in health care facilities to test. Many (this includes men more than women) avoid testing in health facilities because of social visibility, privacy concerns, fear of lack of confidentiality, stigma, discrimination, and also long waiting time, that results in loss of work days. Is it any surprise that 60% of the people living with HIV don’t know that they are infected and continue to spread the infection to their unsuspecting sex partners and children. For those who are tested in facilities, about 30-50% do not return to know their results and never get linked to care.
One practical and bold strategy that may overcome this challenge and expanded access to testing and improve engagement of populations, is an offer of self-testing. Self-testing allows individuals to test themselves in the comfort of their own home. As simple as it sounds, self-testing is in fact a process that assumes a certain level of literacy and self-motivation: one must purchase the test, read and understand the test instructions, perform the test properly, interpret the result accurately, and proactively seek linkages to counseling, confirmatory testing or treatment (as the case may be) by contacting a counsellor or health center. Many African and Asian countries are cautious about introducing and approving self tests, and rightly so. Simply selling self-tests in the stores without clear instructions to test won’t work. The success of a self-testing strategy depends on two key aspects: an accurate result, which can only be obtained if the self-test is correctly performed and interpreted, and proactive linkage seeking to treatment or counselling and availability of timely linkages for anxious self testers. This explains the need for a comprehensive self testing strategy —that is bigger than offering a product, but is tailored to the individuals needs, preferences and circumstances and innovations are needed to support the two key aspects.
Funded by Grand Challenges Canada’s Stars in Global Health Program in 2011, we developed a set of innovations to support these key aspects to create a self-strategy for South Africa. We started out with a global evidence synthesis that summarized the accuracy of oral tests, for self testing. This was published in the Lancet ID (Pant Pai, LID, 2012). Then, we systematically reviewed global evidence on self testing strategies (Pant Pai, Plos Medicine 2013) and plotted all the gaps in the evidence to inform global policy. We had briefly tested a paper application on self testing in Montreal. And then, for this project in South Africa, we focused on developing an integrated innovation in line with the vision of Grand Challenges Canada. We synergized oral non invasive tests with remote counselling by phone and guided (internet-based and paper-based) applications to support crucial aspects of counselling and linkages to care. With the help of our primary collaborator, Professor Keertan Dheda and his team, we tested our strategy in health care workers at the University of Cape Town, South Africa.
Our study results were recently published (DATE) on PLOS One. Overall, all our study participants rated a positive experience with the strategy, and all completed the self-test process. About half of those who tested negative contacted the counselor over the phone. More importantly, all participants that self tested positive for HIV were linked to treatment — a much better performance than facility-based testing.
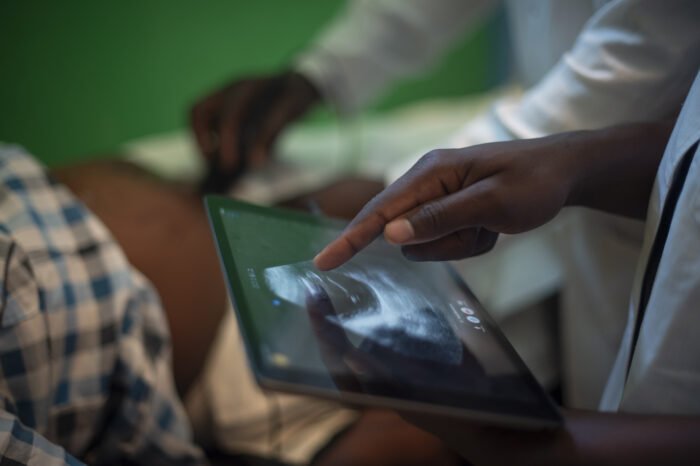
 We then converted the internet application to a smartphone application to take advantage of the increasingly widespread use of mobile phones. This smartphone application called HIVSmart! is available in English, for Android phones but we do aim to convert it to many global languages and platforms. We hope that the smartphone version will be even more engaging and user friendly for the Facebook generation (15-29) and beyond, This generation reports the world’s highest number of incident infections. It will help in reducing operational errors, facilitate linkages with the nearest health facility, and encourage behavior change. Last month, at the World Bank, this strategy was chosen for a global innovation award called ASAP award from Google, PLOS and Wellcome Trust. (http://asap.plos.org).
We then converted the internet application to a smartphone application to take advantage of the increasingly widespread use of mobile phones. This smartphone application called HIVSmart! is available in English, for Android phones but we do aim to convert it to many global languages and platforms. We hope that the smartphone version will be even more engaging and user friendly for the Facebook generation (15-29) and beyond, This generation reports the world’s highest number of incident infections. It will help in reducing operational errors, facilitate linkages with the nearest health facility, and encourage behavior change. Last month, at the World Bank, this strategy was chosen for a global innovation award called ASAP award from Google, PLOS and Wellcome Trust. (http://asap.plos.org).
In line with the vision of Grand Challenges Canada, we are aiming to generate stronger evidence to scale up our innovative self-testing strategy and generate evidence to scale up in ‘at risk’ populations in South Africa. The evidence will not only help South Africa but also similar countries in Sub Saharan Africa, Asia, and Latin America..
We thank Prof Keertan Dheda and his dedicated team of nurses, counsellors, investigators, and researchers for their collaboration, support and faith in the project. We also thank Mr Brian Reid of Orasure Technologies and Mr Jeff Carr of Alere Inc, for their assistance with the rapid tests procurement for this project.
And finally, we thank Grand Challenges Canada for funding our out-of-the-box unconventional solutions. One may have great ideas, but without enlightened funding we cannot push the envelope to meaningfully impact global health.
Follow the author on Twitter @nikkiannike
We encourage you to post your questions and comments about this blog post on our Facebook page Grand Challenges Canada and on Twitter @gchallenges